Do you experience heavy periods,
excessive bleeding, and pelvic pain?
Many of us with fibroids dread our periods and wish we could live life free of discomfort and the fear of accidents. Uterine fibroid embolization or UFE is a simple and effective treatment for fibroids that reduces or eliminates symptoms while letting you keep your uterus. If you are considering hysterectomy, you need to be informed about UFE.
What are the signs that you have fibroids?
- Excessive menstrual bleeding
- Painful and prolonged periods
- Pelvic pain and pressure
- Urinary frequency and loss of bladder control
- Lower back and leg pain
What are uterine fibroids?
Fibroids are muscular tumors that grow in the wall of the uterus (womb). Another medical term for fibroids is leiomyoma or just “myoma.” Fibroids are almost always benign (not cancerous). Fibroids can grow as a single tumor, or there can be many of them in the uterus. They can be as small as an apple seed or as big as a grapefruit. In unusual cases they can become very large.
<1%
Less than 1% of uterine fibroids are cancerous
80%
80% of women will have uterine fibroids before age 50
90%
90% of women will experience significant relief with UFE

Who is at risk?
Most women who have uterine fibroids are between the ages of 35 to 54. African American women are more at risk than other groups. Additional risk factors include a family history of fibroids, early onset of menstruation, obesity, no history of pregnancy, and high blood pressure. Fibroids normally decrease in post-menopausal women.

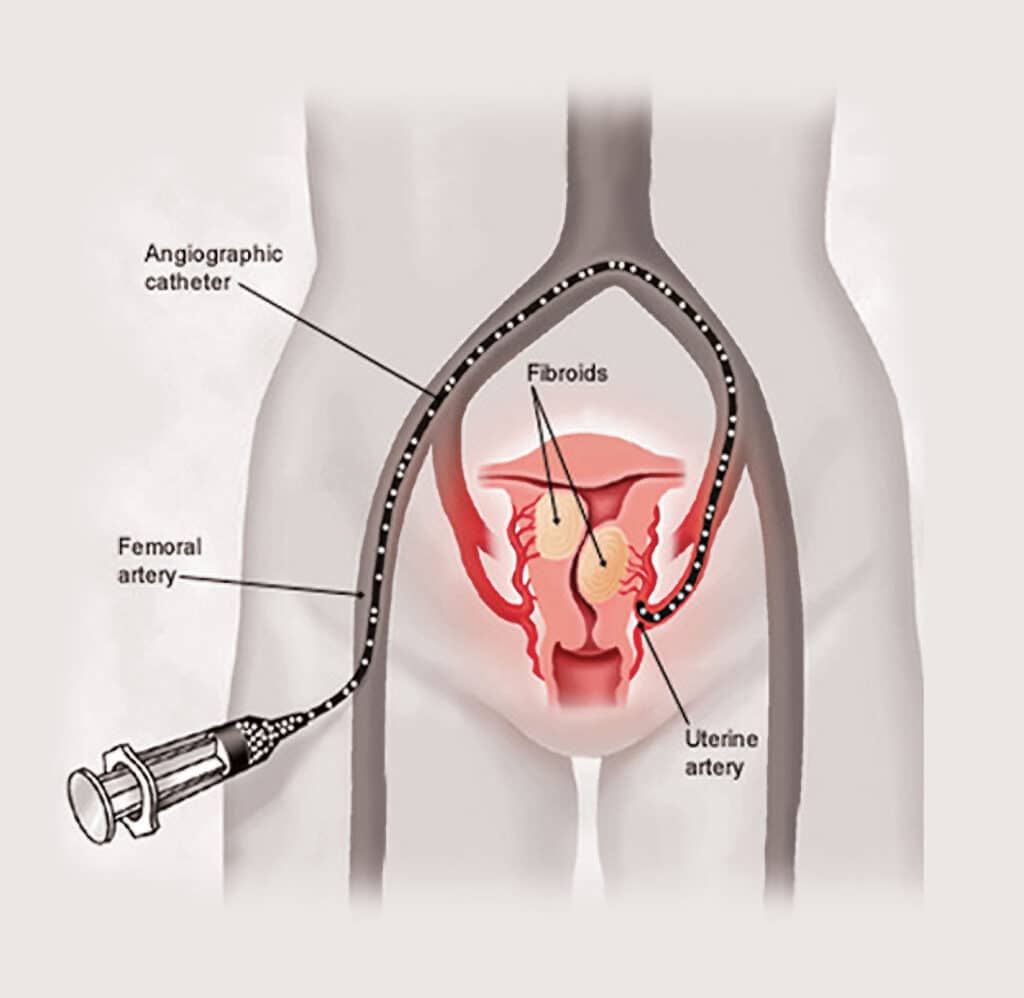
What is uterine fibroid embolization (UFE) treatment?
Uterine fibroid embolization (UFE) is a non-surgical procedure to treat fibroid tumors of the uterus. It begins with a tiny incision in the groin or wrist where a catheter is guided, using a moving X-ray camera, through the circulatory system to the arteries feeding the fibroids. Small spheres of embolic material are injected into the arteries, depriving the fibroids of blood and causing them to shrink over time.

What are the benefits of UFE?
UFE is a nonsurgical therapy that treats all fibroids that are present. This outpatient procedure usually takes less than one hour. Clinical data suggests that patients treated with uterine fibroid embolization return to work and daily activities on average within 7-11 days. Benefits include:
- Decrease in menstrual bleeding from fibroids
- Preservation of the uterus
- Relief of pelvic pain and/or pressure
- Increase in urinary tract function
- More confidence and lower chance of menstrual accidents
- Does not interfere with hormones or other organs
- Overall improvement in physical and emotional well-being

Will my insurance cover this procedure?
Generally, insurance companies will pay for uterine artery embolization if they cover fibroid surgery. Our interventional case coordinators will help you navigate the insurance process.
For more information, please contact interventional case coordinators at (512) 467-9729. Patients and physicians can fax materials to (512) 343-9099.
Coming in from out of town? Visit our “Traveling to Austin” page.


 Back to Top
Back to Top